(especial para SIIC © Derechos reservados)
La contaminación del aire de interiores y de exteriores ha sido considerada un serio problema de salud pública a nivel mundial, el cual se asocia anualmente con alrededor de 7 millones de muertes (4.8 millones asociadas con el aire de exteriores y 2.2 millones con el aire de interiores).
Bruno Rivas Santiago
Columnista Experto de SIIC
Institución:
Instituto Mexicano del Seguro Social Artículos publicados por Bruno Rivas Santiago
César Enrique Rivas Santiago* Gretel Mendoza Almanza** Yamilé López Hernández**
Cátedra CONACYT, Consejo Nacional de Ciencia y Tecnología - Universidad Autónoma de Zacatecas, México*
Cátedra CONACYT, Consejo Nacional de Ciencia y Tecnología - Universidad Autónoma de Zacatecas**
|
Recepción del artículo 19 de Abril, 2019 |
Aprobación 29 de Agosto, 2019 |
|
Primera edición 3 de Septiembre, 2019 |
Segunda edición, ampliada y corregida 2 de Febrero, 2024 |
|
|
|
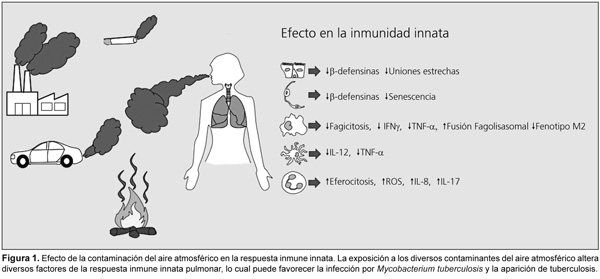
La contaminación del aire de interiores y de exteriores ha sido considerada un serio problema de salud pública a nivel mundial, el cual se asocia anualmente con alrededor de 7 millones de muertes (4.8 millones asociadas con el aire de exteriores y 2.2 millones con el aire de interiores). Entre las principales razones ligadas a estas muertes se encuentran: enfermedad pulmonar obstructiva crónica, neumonía, cardiopatía isquémica y cáncer de pulmón. Además, estudios epidemiológicos han asociado la exposición a este tipo de contaminantes con mayor susceptibilidad para la aparición de enfermedades infecciosas y no infecciosas. Entre las enfermedades infecciosas, una de las más importantes es la tuberculosis, la cual, durante el transcurso de los años, ha empeorado con el surgimiento de cepas resistentes a múltiples fármacos, así como por la asociación con otras afecciones como la diabetes mellitus tipo 2 y el síndrome de inmunodeficiencia adquirida (sida). A pesar del esfuerzo realizado por la Organización Mundial de la Salud (OMS) por detener esta epidemia, aún existen anualmente un gran número de muertes causadas por esta enfermedad: alrededor de 1.7 millones a nivel mundial. En esta revisión se hará un breve resumen de los efectos que tiene la exposición a la contaminación del aire de interiores y de exteriores en la respuesta inmune innata en contra de la tuberculosis, y cómo estas alteraciones pueden estar ligadas a la aparición de tuberculosis pulmonar. contaminación del aire, tuberculosis, inmunidad, inmunidad innata, material particulado, SIDA
Artículo completo
LA CONTAMINACION DEL AIRE ATMOSFERICO EN LA RESPUESTA INMUNE INNATA ANTIMICOBACTERIANA
1. Global tuberculosis report 2017. Geneva: World Health Organization; 2017. 2. Ferrara G, et al. Risk factors associated with pulmonary tuberculosis: smoking, diabetes and anti-TNFalpha drugs. Curr Opin Pulm Med 18(3):233-240, 2012. 3. Gutiérrez EB, et al. Active tuberculosis and Mycobacterium tuberculosis latent infection in patients with HIV/AIDS. HIV Med 10(9):564-572, 2009. 4. Lin HH, Ezzati M, Murray M. Tobacco smoke, indoor air pollution and tuberculosis: a systematic review and meta-analysis. PLoS Med 4(1): e20, 2007. 5. Zielonka TM. Risk factors for tuberculosis and specific manifestations of disease. Przegl Epidemiol 68(4):637-643, 2014. 6. Jafta N, et al. Childhood tuberculosis and exposure to indoor air pollution: a systematic review and meta-analysis. Int J Tuberc Lung Dis 19(5):596-602, 2015. 7. Smith GS, et al. Particulate air pollution and susceptibility to the development of pulmonary tuberculosis disease in North Carolina: an ecological study. Int J Environ Health Res 24(2):103-112, 2014. 8. WHO: 7 million premature deaths annually linked to air pollution. Geneva: World Health Organization; 2014. 9. Liu CH, Liu H, Ge B. Innate immunity in tuberculosis: host defense vs pathogen evasion. Cell Mol Immunol 14(12):963-975, 2017. 10. Mayer AK, et al. Differential recognition of TLR-dependent microbial ligands in human bronchial epithelial cells. J Immunol 178(5):3134-3142, 2007. 11. Boggaram V, et al. Early secreted antigenic target of 6 kDa (ESAT-6) protein of Mycobacterium tuberculosis induces interleukin-8 (IL-8) expression in lung epithelial cells via protein kinase signaling and reactive oxygen species. J Biol Chem 288(35):25500-25511, 2013. 12. Rivas-Santiago B, et al. Human {beta}-defensin 2 is expressed and associated with Mycobacterium tuberculosis during infection of human alveolar epithelial cells. Infect Immun 73(8):4505-4511, 2005. 13. Oppenheim JJ, et al. Roles of antimicrobial peptides such as defensins in innate and adaptive immunity. Ann Rheum Dis 62(Suppl 2):17-21, 2003. 14. Prendergast KA, Kirman JR. Dendritic cell subsets in mycobacterial infection: control of bacterial growth and T cell responses. Tuberculosis (Edinb) 93(2):115-122, 2013. 15. Bollampalli VP, et al. BCG Skin Infection Triggers IL-1R-MyD88-Dependent Migration of EpCAMlow CD11bhigh Skin Dendritic cells to Draining Lymph Node During CD4+ T-Cell Priming. PLoS Pathog 11(10):e1005206, 2015. 16. Green AM, Difazio R, Flynn JL. IFN-gamma from CD4 T cells is essential for host survival and enhances CD8 T cell function during Mycobacterium tuberculosis infection. J Immunol 190(1):270-277, 2013. 17. Chua J, et al. A tale of two lipids: Mycobacterium tuberculosis phagosome maturation arrest. Curr Opin Microbiol 7(1):71-77, 2004. 18. Deretic V, et al. Mycobacterium tuberculosis inhibition of phagolysosome biogenesis and autophagy as a host defence mechanism. Cell Microbiol 8(5):719-727, 2006. 19. Dahl KE, et al. Selective induction of transforming growth factor beta in human monocytes by lipoarabinomannan of Mycobacterium tuberculosis. Infect Immun 64(2):399-405, 1996. 20. Hickman SP, Chan J, Salgame P. Mycobacterium tuberculosis induces differential cytokine production from dendritic cells and macrophages with divergent effects on naive T cell polarization. J Immunol 168(9):4636-4642, 2002. 21. Mayer-Barber KD, et al. Innate and adaptive interferons suppress IL-1alpha and IL-1beta production by distinct pulmonary myeloid subsets during Mycobacterium tuberculosis infection. Immunity 35(6):1023-1034, 2011. 22. Roca FJ, Ramakrishnan L. TNF dually mediates resistance and susceptibility to mycobacteria via mitochondrial reactive oxygen species. Cell 153(3):521-534, 2013. 23. Nigou J, et al. Mannosylated lipoarabinomannans inhibit IL-12 production by human dendritic cells: evidence for a negative signal delivered through the mannose receptor. J Immunol 166(12):7477-7485, 2001. 24. Tufariello JM, Chan J, Flynn JL. Latent tuberculosis: mechanisms of host and bacillus that contribute to persistent infection. Lancet Infect Dis 3(9): 578-590, 2003. 25. Kwan CK, Ernst JD. HIV and tuberculosis: a deadly human syndemic. Clin Microbiol Rev 24(2):351-376, 2011. 26. Restrepo BI. Diabetes and Tuberculosis. Microbiol Spectr 4(6), 2016. 27. Koyanagi A, et al. Depression comorbid with tuberculosis and its impact on health status: cross-sectional analysis of community-based data from 48 low- and middle-income countries. BMC Med 15(1):209, 2017. 28. Zhu S, et al. Ambient air pollutants are associated with newly diagnosed tuberculosis: A time-series study in Chengdu, China. Sci Total Environ 631-632:47-55, 2018. 29. Lai TC, et al. Ambient air pollution and risk of tuberculosis: a cohort study. Occup Environ Med 73(1):56-61, 2016. 30. Royal College of Physicians of London. Every breath we take: the lifelong impact of air pollution: report of a working party. London: Royal College of Physicians of London; 2016. Pp. 106. 31. WHO, 7 million premature deaths annually linked to air pollution. World Health Organization: Geneva, Switzerland; 2016. 32. Dockery DW, et al. An association between air pollution and mortality in six U.S. cities. N Engl J Med 329(24):1753-1759, 1993. 33. Pope CA. 3rd, et al. Particulate air pollution as a predictor of mortality in a prospective study of U.S. adults. Am J Respir Crit Care Med 151(3 Pt 1):669-674, 1995. 34. Brunekreef B, et al. Effects of long-term exposure to traffic-related air pollution on respiratory and cardiovascular mortality in the Netherlands: the NLCS-AIR study. Res Rep Health Eff Inst 139:5-71, 2009. 35. Hoek G, et al. Ass ociation between mortality and indicators of traffic-related air pollution in the Netherlands: a cohort study. Lancet 360(9341):1203-1209, 2002. 36. Avino P, et al. Second-hand aerosol from tobacco and electronic cigarettes: Evaluation of the smoker emission rates and doses and lung cancer risk of passive smokers and vapers. Sci Total Environ 642:137-147, 2018. 37. Nyberg F, et al. Urban air pollution and lung cancer in Stockholm. Epidemiology 11(5):487-495, 2000. 38. Smith GS, et al. Air Pollution and Pulmonary Tuberculosis: A Nested Case-Control Study among Members of a Northern California Health Plan. Environ Health Perspect 124(6):761-768, 2016. 39. Ezzati M, Kammen DM. Quantifying the effects of exposure to indoor air pollution from biomass combustion on acute respiratory infections in developing countries. Environ Health Perspect 109(5):481-488, 2001. 40. Smith KR. Indoor air pollution in developing countries: recommendations for research. Indoor Air 12(3):198-207, 2002. 41. Oxlade O, Murray M. Tuberculosis and poverty: why are the poor at greater risk in India? PLoS One 7(11):e47533, 2012. 42. Coker R, et al. Risk factors for pulmonary tuberculosis in Russia: case-control study. BMJ 332(7533):85-87, 2006. 43. Kashyap RS, et al. Impact of socioeconomic status and living condition on latent tuberculosis diagnosis among the tribal population of Melghat: A cohort study. Lung India 33(4):372-380, 2016. 44. Ozturk AB, Kilicaslan Z, Issever H. Effect of smoking and indoor air pollution on the risk of tuberculosis: smoking, indoor air pollution and tuberculosis. Tuberk Toraks 62(1):1-6, 2014. 45. Elf JL, et al. The association of household fine particulate matter and kerosene with tuberculosis in women and children in Pune, India. Occup Environ Med 76(1):40-47, 2019. 46. Elf JL, et al. Indoor air pollution from secondhand tobacco smoke, solid fuels, and kerosene in homes with active tuberculosis disease in South Africa. BMC Res Notes 10(1):591, 2017. 47. Kurmi OP, et al. Tuberculosis risk from exposure to solid fuel smoke: a systematic review and meta-analysis. J Epidemiol Community Health 68(12):1112-1118, 2014. 48. Sehgal M, Rizwan SA, Krishnan A. Disease burden due to biomass cooking-fuel-related household air pollution among women in India. Glob Health Action 7:25326, 2014. 49. Swiston JR, et al. Wood smoke exposure induces a pulmonary and systemic inflammatory response in firefighters. Eur Respir J 32(1):129-138, 2008. 50. Kulkarni NS, et al. Carbon loading of alveolar macrophages in adults and children exposed to biomass smoke particles. Sci Total Environ 345(1-3):23-30, 2005. 51. Fullerton DG, et al. Domestic smoke exposure is associated with alveolar macrophage particulate load. Trop Med Int Health 14(3):349-354, 2009. 52. Rylance J, et al. Household air pollution causes dose-dependent inflammation and altered phagocytosis in human macrophages. Am J Respir Cell Mol Biol 52(5):584-593, 2015. 53. Kurmi OP, et al. Oxidative potential of smoke from burning wood and mixed biomass fuels. Free Radic Res 47(10):829-835, 2013. 54. Nishimura Y, et al. Exposure to negatively charged-particle dominant air-conditions on human lymphocytes in vitro activates immunological responses. Immunobiology 220(12):1359-1368, 2015. 55. Rock KL. Pathobiology of inflammation to cell death. Biol Blood Marrow Transplant 15(1 Suppl):137-138, 2009. 56. Lopez-Hernandez Y, et al. Tuberculosis and cigarette smoke exposure: An update of in vitro and in vivo studies. Exp Lung Res 44(2):113-126,2018. 57. Bishwakarma R, et al. Epidemiologic link between tuberculosis and cigarette/biomass smoke exposure: Limitations despite the vast literature. Respirology 20(4):556-568, 2015. 58. van Zyl-Smit RN, et al. Cigarette smoke impairs cytokine responses and BCG containment in alveolar macrophages. Thorax 69(4):363-370, 2014. 59. Harris JO, Gonzalez-Rothi RJ. Abnormal phagolysosome fusion in pulmonary alveolar macrophages of rats exposed chronically to cigarette smoke. Am Rev Respir Dis 130(3):467-471, 1984. 60. Shaykhiev R, et al. Smoking-dependent reprogramming of alveolar macrophage polarization: implication for pathogenesis of chronic obstructive pulmonary disease. J Immunol 183(4):2867-2883, 2009. 61. Fu X, et al. M2 polarized macrophages induced by CSE promote proliferation, migration, and invasion of alveolar basal epithelial cells. Int Immunopharmacol 28(1):666-674, 2015. 62. Monick MM, et al. Identification of an autophagy defect in smokers' alveolar macrophages. J Immunol 185(9):5425-5435, 2010. 63. Bai X, et al. Nicotine Impairs Macrophage Control of Mycobacterium tuberculosis. Am J Respir Cell Mol Biol 57(3):324-333, 2017. 64. Minematsu N, Blumental-Perry A, Shapiro SD. Cigarette smoke inhibits engulfment of apoptotic cells by macrophages through inhibition of actin rearrangement. Am J Respir Cell Mol Biol 44(4):474-482, 2011. 65. Shang S, et al. Cigarette smoke increases susceptibility to tuberculosis--evidence from in vivo and in vitro models. J Infect Dis 203(9):1240-1248, 2011. 66. Shaler CR, et al. Continuous and discontinuous cigarette smoke exposure differentially affects protective Th1 immunity against pulmonary tuberculosis. PLoS One 8(3):e59185, 2013. 67. Levings MK, Schrader JW. IL-4 inhibits the production of TNF-alpha and IL-12 by STAT6-dependent and -independent mechanisms. J Immunol 162(9):5224-5229, 1999. 68. Corleis B, et al. Escape of Mycobacterium tuberculosis from oxidative killing by neutrophils. Cell Microbiol 14(7):1109-1121, 2012. 69. Lowe DM, et al. Neutrophils in tuberculosis: friend or foe? Trends Immunol 33(1):14-25, 2012. 70. Blidberg K, et al. Increased neutrophil migration in smokers with or without chronic obstructive pulmonary disease. Respirology 17(5):854-860, 2012. 71. Harrison OJ, et al. Airway infiltration of CD4+ CCR6+ Th17 type cells associated with chronic cigarette smoke induced airspace enlargement. Immunol Lett 121(1):13-21, 2008. 72. Eum SY, et al. Neutrophils are the predominant infected phagocytic cells in the airways of patients with active pulmonary TB. Chest 137(1):122-128, 2010. 73. Nuvolone D, Petri D, Voller F. The effects of ozone on human health. Environ Sci Pollut Res Int 25(9):8074-8088, 2018. 74. Kim KH, Kabir E, Kabir S. A review on the human health impact of airborne particulate matter. Environ Int 74:136-143, 2015. 75. Wei Q, et al. Short-term exposure to sulfur dioxide and the risk of childhood hand, foot, and mouth disease during different seasons in Hefei, China. Sci Total Environ 658:116-121, 2019. 76. Popovic I, et al. A systematic literature review and critical appraisal of epidemiological studies on outdoor air pollution and tuberculosis outcomes. Environ Res 170:33-45, 2019. 77. Sohn M, et al. Association of social deprivation and outdoor air pollution with pulmonary tuberculosis in spatiotemporal analysis. Int J Environ Health Res 2019:1-11, 2019. 78. Liu Y, et al. Ambient Air Pollution Exposures and Newly Diagnosed Pulmonary Tuberculosis in Jinan, China: A Time Series Study. Sci Rep 8(1):17411, 2018. 79. Hwang SS, et al. Impact of outdoor air pollution on the incidence of tuberculosis in the Seoul metropolitan area, South Korea. Korean J Intern Med 29(2):183-190, 2014. 80. Peng Z, et al. Long-term exposure to ambient air pollution and mortality in a Chinese tuberculosis cohort. Sci Total Environ 580:1483-1488, 2017. 81. Jassal MS, Bakman I, Jones B. Correlation of ambient pollution levels and heavily-trafficked roadway proximity on the prevalence of smear-positive tuberculosis. Public Health 127(3):268-274, 2013. 82. Chen KY, et al. Particulate matter is associated with sputum culture conversion in patients with culture-positive tuberculosis. Ther Clin Risk Manag 12:41-46, 2016. 83. Sierra-Vargas MP, Teran LM. Air pollution: impact and prevention. Respirology 17(7):1031-1038, 2012. 84. Nel A. Atmosphere. Air pollution-related illness: effects of particles. Science 308(5723):804-806, 2005. 85. Rivas-Santiago CE, et al. Air pollution particulate matter alters antimycobacterial respiratory epithelium innate immunity. Infect Immun 83(6):2507-2517, 2015. 86. Chen X, et al. Urban particulate matter (PM) suppresses airway antibacterial defence. Respir Res 19(1):5, 2018. 87. Vargas Buonfiglio LG, et al. Effects of Coal Fly Ash Particulate Matter on the Antimicrobial Activity of Airway Surface Liquid. Environ Health Perspect 125(7):077003,017. 88. Zhang Y, et al. Suppression of Neutrophil Antimicrobial Functions by Total Particulate Matter From Cigarette Smoke. Front Immunol 9:2274, 2018. 89. He M, et al. PM2.5-induced lung inflammation in mice: Differences of inflammatory response in macrophages and type II alveolar cells. J Appl Toxicol 37(10):1203-1218, 2017. 90. Musah S, DeJarnett N, Hoyle GW. Tumor necrosis factor-alpha mediates interactions between macrophages and epithelial cells underlying proinflammatory gene expression induced by particulate matter. Toxicology 299(2-3): 125-132, 2012. 91. Castaneda AR, et al. Ambient particulate matter activates the aryl hydrocarbon receptor in dendritic cells and enhances Th17 polarization. Toxicol Lett 292:85-96, 2018. 92. Shen H,Chen ZW. The crucial roles of Th17-related cytokines/signal pathways in M. tuberculosis infection. Cell Mol Immunol 15(3):216-225, 2018. 93. Yu Y, et al. Effects of ambient air pollution from municipal solid waste landfill on children's non-specific immunity and respiratory health. Environ Pollut 236:382-390, 2018. 94. Yang J, et al. Changes in gene expression in lungs of mice exposed to traffic-related air pollution. Mol Cell Probes 39:33-40, 2018. 95. Kehrl HR, et al. Ozone exposure increases respiratory epithelial permeability in humans. Am Rev Respir Dis 135(5):1124-1128, 1987. 96. Que LG, et al. Pulmonary function, bronchial reactivity, and epithelial permeability are response phenotypes to ozone and develop differentially in healthy humans. J Appl Physiol (1985) 111(3):679-687, 2011. 97. Lee D, et al. Disruption of tracheobronchial airway growth following postnatal exposure to ozone and ultrafine particles. Inhal Toxicol 23(9):520-531, 2011. 98. Gilmour MI, et al. Suppression and recovery of the alveolar macrophage phagocytic system during continuous exposure to 0.5 ppm ozone. Exp Lung Res 17(3):547-558, 1991. 99. Mikerov AN, et al. Impact of ozone exposure on the phagocytic activity of human surfactant protein A (SP-A) and SP-A variants. Am J Physiol Lung Cell Mol Physiol 294(1):L121-130, 2008. 100. Arsalane K, et al. Ozone stimulates synthesis of inflammatory cytokines by alveolar macrophages in vitro. Am J Respir Cell Mol Biol 13(1):60-68, 1995. 101. Manzer R, et al. Ozone exposure of macrophages induces an alveolar epithelial chemokine response through IL-1alpha. Am J Respir Cell Mol Biol 38(3):318-323, 2008. 102. Kleeberger SR, et al. Toll-like receptor 4 mediates ozone-induced murine lung hyperpermeability via inducible nitric oxide synthase. Am J Physiol Lung Cell Mol Physiol 280(2):L326-333, 2001. 103. Belianin II, et al. Use of dissolved ozone in the treatment of experimental tuberculosis in mice. Probl Tuberk Bolezn Legk 10:36-39, 2004. |
|
|
Está expresamente prohibida la redistribución y la redifusión de todo o parte de los contenidos de la Sociedad Iberoamericana de Información Científica (SIIC) S.A. sin previo y expreso consentimiento de SIIC. |